What is rheumatoid arthritis?
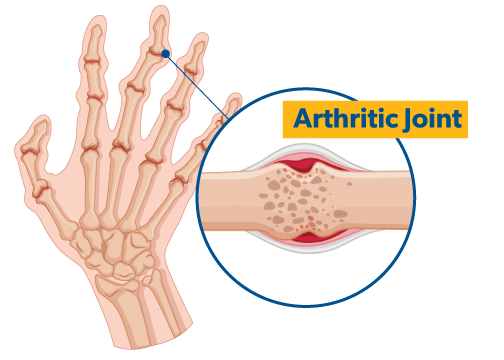 Rheumatoid arthritis (RA) is a common, autoimmune disease that causes inflammation and pain in multiple joints of the body.
Rheumatoid arthritis (RA) is a common, autoimmune disease that causes inflammation and pain in multiple joints of the body.
An autoimmune disease happens when the body’s immune system, which normally functions to protect against infections, attacks healthy tissues by mistake. In rheumatoid arthritis, the immune system attacks the lining of joints leading to inflammation, swelling, pain, and stiffness. Inflammation is like a fire. It can spread throughout the body and damage areas it touches.
If the fire is not put out, it can lead to damage of the joints and loss of function. The “fire” of inflammation can also affect other organs, such as the nerves, eyes, skin, lungs or heart.
The cause of rheumatoid arthritis is still unknown. There is no cure for rheumatoid arthritis but there are many effective ways to “put out the fire,” including medications and other therapies that help the symptoms and results of inflammation.
Treatment
Finding treatment options that are effective at relieving pain and reducing inflammation are important to preserve joint health. Thinking of inflammation like a “fire” burning in the joints means any fire left unattended may cause damage. Once a joint is damaged it cannot be fixed other than through surgery. Just as you would try to put out a fire in your home with a fire extinguisher before it spreads, you want to put out the inflammation of rheumatoid arthritis as quickly and as safely as possible.
It is important to treat rheumatoid arthritis as early as possible as research has confirmed that this improves the long-term outcomes and quality of life of people living with rheumatoid arthritis.
Medication
There are a variety of medications that can be used to help treat symptoms of pain and inflammation caused by rheumatoid arthritis, though not all medications are the same, or work in the same way. There are three main categories of medications that are often used to help treat rheumatoid arthritis or its symptoms.
Non-steroidal anti-inflammatory medications (NSAIDs)
 NSAIDs are a very common type of anti-inflammatory medication. Some forms of NSAIDs are available over the counter, such as ibuprofen, while other forms of NSAIDs require a prescription. NSAIDs are often a first-line treatment (what someone tries first) to help treat pain and inflammation from rheumatoid arthritis.
NSAIDs are a very common type of anti-inflammatory medication. Some forms of NSAIDs are available over the counter, such as ibuprofen, while other forms of NSAIDs require a prescription. NSAIDs are often a first-line treatment (what someone tries first) to help treat pain and inflammation from rheumatoid arthritis.
NSAIDs work by helping the body to block the production of a hormone-like chemical called prostaglandin. The body naturally produces prostaglandins to help regulate many systems in the body, including responding to acute injuries or pain. Prostaglandins contribute to inflammation and redness at the site of injury. However, for a more chronic condition like arthritis, too much prostaglandin production can lead to chronic inflammation and pain around the affected joints. NSAIDs help by temporarily blocking the body’s ability to produce prostaglandins and help reduce the amount of inflammation and pain. It is always best to speak with your doctor or pharmacist about how and when to take NSAIDs. Taking NSAIDs at the first sign of a flare, before the body can produce excess prostaglandins, may be more effective than starting it in the middle of a flare.
While NSAIDs can ease the symptoms of rheumatoid arthritis, it is important to note they are a temporary option that help with symptoms but once stopped, symptoms may return. NSAIDs do not control the underlying problem, which is an overactive immune system, which is why your rheumatologist will recommend a rheumatoid arthritis specific treatment.
Disease-modifying anti-rheumatic drugs (DMARDs)
DMARDs are a class of arthritis medications that are designed to suppress and modify the immune system’s inflammation response. They help put out the “fire” of excessive inflammation throughout the body. These medications are often taken long-term and can take weeks before their effects are felt. Since each DMARD can affect different people differently, sometimes a combination of medications (known as combination therapy) is needed to be most effective at relieving symptoms and controlling the disease.
Biologics and biosimilars are a form of DMARD created from living cells. Each biologic or biosimilar works to better target the immune system to stop inflammation and prevent or slow disease progression.
Janus Kinase or JAK inhibitors are another type of DMARD, belonging to a family of drugs called tsDMARDs (targeted synthetic disease-modifying anti-rheumatic drugs). These drugs interfere with the activity of specific enzymes in the body (e.g., JAK1, JAK2, JAK3, TYK2) to reduce the body’s overactive immune response by interrupting how signals are sent throughout the cells.
To learn more about each medication, consult Arthritis Medications – A Reference Guide or watch the video Biologics, Biosimilars and JAK Inhibitors.
Medical treatment plans
Arthritis medications are designed to control the disease, to slow its progression and to help manage symptoms. These medications can be very complex, so it’s important to talk with your doctor or pharmacist about any questions you may have, or for more detailed explanations specific to your health and wellness.
Common medication therapies
Medication therapies typically include 1 to 3 disease-modifying anti-rheumatic drugs (DMARDs).
- Most common: methotrexate (pills or injections weekly) with folic acid supplements to help reduce potential side effects such as mouth sores or gastrointestinal upset.
- Sometimes: sulfasalazine, hydroxychloroquine, leflunomide, or others will also be prescribed in combination with methotrexate.
You can expect follow-up lab tests and frequent monitoring to assess the effectiveness and side effects of your treatment.
Your rheumatologist can refine DMARD treatment to better control rheumatoid arthritis for advanced treatments:
- Switch to a different DMARD
- Add DMARDs in combination
Medication options for short term use or flares
For short-term use or flare-ups, treatment may include:
- Steroid pills, or corticosteroid injections in affected joints or intra-muscularly
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Non-opioid painkillers (analgesics)
Biologics or other targeted treatments
Your rheumatologist can add biologics or other targeted treatments:
- TNF inhibitors (adalimumab, certolizumab pegol, etanercept, golimumab, infliximab)
- JAK inhibitors (tofacitinib, baricitinib, upadacitinib)
- IL-6 inhibitors (tocilizumab, sarilumab)
- Selective T cell co-stimulation modulator (abatacept)
- Selective B cell depletion (rituximab)
You may need to be screened for tuberculosis or other infections before starting medications. Your treatment may require injections under the skin or infusions into a vein.
There is an ongoing need for you to visit your rheumatologist to consider the use of different biologic or targeted treatment until your rheumatoid arthritis is well controlled.
Managing stress
 Finding a medication or combination of medications that works for you may take some time and may require trying a few different medications before something works. This process may feel frustrating, discouraging, or overwhelming. It is okay to feel this way, but if you notice your thoughts or feelings are causing you to feel sad more often, or you have difficulty concentrating on other things that are important to you, let your doctor or healthcare team know. It’s important to take care of all aspects of your health, including your mental health too.
Finding a medication or combination of medications that works for you may take some time and may require trying a few different medications before something works. This process may feel frustrating, discouraging, or overwhelming. It is okay to feel this way, but if you notice your thoughts or feelings are causing you to feel sad more often, or you have difficulty concentrating on other things that are important to you, let your doctor or healthcare team know. It’s important to take care of all aspects of your health, including your mental health too.
Managing a new diagnosis, chronic pain and health issues can take a toll on mental health. The Mental Health Resource Hub can help you identify ways to better cope.
Surgery
Surgery is not common for inflammatory arthritis but may be necessary after many years of severe disease. Surgery may be needed to relieve pain, straighten out a bent or deformed joint, restore mobility or replace a damaged joint. Sometimes the tendons and ligaments around joints, such as the hips, may need to be lengthened. A surgeon may also be asked to make recommendations on splinting and rehabilitation.
Read about others experiences with joint surgery.
Symptoms and Diagnosis
 The symptoms of rheumatoid arthritis vary widely from person to person. In many cases, it can start in a few joints then spread to other joints over a few weeks to months. Rheumatoid arthritis can also progress extremely quickly, with some people reporting waking up one morning just not able to get out of bed.
The symptoms of rheumatoid arthritis vary widely from person to person. In many cases, it can start in a few joints then spread to other joints over a few weeks to months. Rheumatoid arthritis can also progress extremely quickly, with some people reporting waking up one morning just not able to get out of bed.
The earliest symptoms of rheumatoid arthritis can be non-specific, including feeling unwell or tired, soreness around joints and muscles, low-grade fever, and weight loss or poor appetite. As time goes on, rheumatoid arthritis can involve more and more joints on both sides of the body, often in a symmetrical pattern.
More than 250,000 people living in Canada have rheumatoid arthritis and people can develop symptoms at any age. Children can have a form of rheumatoid arthritis called Juvenile Rheumatoid Arthritis (JRA).
Females are affected by rheumatoid arthritis two to three times more often than males. Though the reasons for this are not entirely clear, the connection between hormones and the immune system, as well as genetics associated with the X chromosome are being considered as possible contributing factors. The prevalence and impact of rheumatoid arthritis in people who are intersex or trans is largely unknown, as is the impact of gender-affirming hormone therapy.
There is no cure for rheumatoid arthritis, however, people who receive a diagnosis and begin treatment early are more likely to limit damage to their joints and continue to live active lives.
Early signs and symptoms
Rheumatoid arthritis usually starts over a period of weeks to months, with more joints becoming affected over time. You should see your doctor if you experience one or more of the following symptoms for more than six weeks:
- Pain or stiffness in multiple joints
- “Gelling” or stiffness of joints, especially in the morning, that lasts 30 minutes or more
- Warmth or redness over joints
- Reduced ability to move the joints (such as difficulty making a fist, twisting objects, opening objects, climbing stairs)
- Fever, fatigue, weight loss or decreased appetite
- Lumpy growths that form under your skin, most commonly on the elbows, hands or feet
Any joint can be affected in rheumatoid arthritis, but the joints most commonly involved include:
- Knuckles and small joints of the hand
- Toes
- Wrists
- Elbows
- Shoulders
- Knees
- Ankles
Watch the video series: Symptoms to Diagnosis
 |
 |
 |
| Recognizing the first signs of arthritis | What is a rheumatologist? | What to expect when seeing a rheumatologist |
What are the risk factors for rheumatoid arthritis?
The exact causes of rheumatoid arthritis are unknown, but research has shown there are several things that may contribute:
Family/genetic history
Some people who develop rheumatoid arthritis have specific genes that may predispose them to developing rheumatoid arthritis, though this does not necessarily mean you will develop rheumatoid arthritis if you carry these genes.
Sex
Rheumatoid arthritis is two to three times more likely to affect females than males.
Hormones
Some hormonal changes appear to be linked to rheumatoid arthritis. Hormone changes during and after pregnancy, during breast or chest feeding and even oral contraception use may be linked to the development of rheumatoid arthritis or may relieve or trigger rheumatoid arthritis symptoms. There is not currently enough research to indicate how symptoms of rheumatoid arthritis in trans people taking hormone replacement therapy (HRT) might be impacted, or if taking HRT would lessen or worsen symptoms of rheumatoid arthritis.
Age
Rheumatoid arthritis can affect people any age, but the risk of developing the disease increases with age, commonly developing between 40 and 60 years.
Environment
Infection can trigger rheumatoid arthritis in people who have genetic links to the disease. However, it is important to remember that you cannot catch or spread rheumatoid arthritis and it is not contagious.
Traumatic events
Major trauma or physical or emotional stress can also act as a trigger for symptom onset.
Smoking
Numerous studies have shown that cigarette smoking is the strongest environmental risk for the development of rheumatoid arthritis and for having a more severe form of the disease.
Gum disease
 Gum disease can change your immune responses and make you more susceptible to inflammatory arthritis. While it is not yet known if gum disease can cause rheumatoid arthritis, or if having rheumatoid arthritis can cause gum disease, gum disease is more common in people who have rheumatoid arthritis, and vice versa. Gum disease is also associated with having more severe rheumatoid arthritis. Good dental hygiene is important for everyone, but especially if you have symptoms of rheumatoid arthritis, another inflammatory condition, or have symptoms of gum disease. Gum disease is also a risk factor for many other conditions, such as heart disease, diabetes, and kidney disease.
Gum disease can change your immune responses and make you more susceptible to inflammatory arthritis. While it is not yet known if gum disease can cause rheumatoid arthritis, or if having rheumatoid arthritis can cause gum disease, gum disease is more common in people who have rheumatoid arthritis, and vice versa. Gum disease is also associated with having more severe rheumatoid arthritis. Good dental hygiene is important for everyone, but especially if you have symptoms of rheumatoid arthritis, another inflammatory condition, or have symptoms of gum disease. Gum disease is also a risk factor for many other conditions, such as heart disease, diabetes, and kidney disease.
Rheumatoid arthritis flares
 A flare is a sudden onset of rheumatoid arthritis symptoms after having a period of time either without symptoms (sometimes called remission), or with less bothersome symptoms. Sometimes symptoms of rheumatoid arthritis will flare (come on suddenly) during a time of stress, illness or life changes. Since no two people are the same, it can be helpful to track what type of symptoms you have during a flare, and how long they last. This will help you discuss symptoms with your doctor and find ways to manage symptoms when they appear. In general, a flare is temporary and should only last a few weeks. If symptoms last longer, speak with your doctor.
A flare is a sudden onset of rheumatoid arthritis symptoms after having a period of time either without symptoms (sometimes called remission), or with less bothersome symptoms. Sometimes symptoms of rheumatoid arthritis will flare (come on suddenly) during a time of stress, illness or life changes. Since no two people are the same, it can be helpful to track what type of symptoms you have during a flare, and how long they last. This will help you discuss symptoms with your doctor and find ways to manage symptoms when they appear. In general, a flare is temporary and should only last a few weeks. If symptoms last longer, speak with your doctor.
How is rheumatoid arthritis diagnosed?
An accurate diagnosis is very important because there are many ways to treat and manage rheumatoid arthritis. Early diagnosis and treatment can reduce the pain and disability associated with this disease.
There is no single test to determine if you have rheumatoid arthritis. If you have signs and symptoms of rheumatoid arthritis, your doctor will examine your joints and take your medical history. If indicated, a blood tests that detect inflammation may be ordered that may help confirm the diagnosis. Your healthcare provider may also order X-rays to look for any signs of joint damage. If your family doctor suspects you have rheumatoid arthritis, you will be referred to a specialist called a rheumatologist.
Rheumatologist visit and tests
Your appointment with a rheumatologist will include:
- A review of your medical history, including your new joint symptoms.
- A general physical examination.
- A joint examination and counting of tender and swollen joints to determine how many are inflamed
- An examination of your skin, heart, lungs to see if the inflammation affects any other areas of your body.
- Ordering any additional blood tests and imaging (e.g., X-rays or ultrasound) that may help with making a diagnosis or determining the correct path of treatment for your symptoms.
It can take some time to identify the exact cause of your symptoms and confirm a diagnosis. While some people may be diagnosed right away, for most people, it may take multiple visits and several tests before your rheumatologist and other members of your healthcare team are able to provide you with a diagnosis and discuss treatment options with you.
Blood Tests
 Ordering a blood test is a common step in the diagnostic process, though it only makes up one part of the many factors doctors consider when making a diagnosis of rheumatoid arthritis. Rheumatologists check the antibody levels of two different proteins that are often elevated in people with rheumatoid arthritis. The first is called rheumatoid factor, and the other is a set of antibodies called anti-citrullinated protein antibodies (ACPAs), or more specifically, anti-cyclic citrullinated peptide antibodies (anti-CCPs).
Ordering a blood test is a common step in the diagnostic process, though it only makes up one part of the many factors doctors consider when making a diagnosis of rheumatoid arthritis. Rheumatologists check the antibody levels of two different proteins that are often elevated in people with rheumatoid arthritis. The first is called rheumatoid factor, and the other is a set of antibodies called anti-citrullinated protein antibodies (ACPAs), or more specifically, anti-cyclic citrullinated peptide antibodies (anti-CCPs).
Rheumatoid Factor and Anti-Cyclic Citrullinated Peptide Antibodies (Anti-CCPs)
Rheumatoid factor and anti-CCPs are both antibodies made by the immune system that can sometimes attack healthy tissue instead of germs and harmful bacteria. When there are more of these antibodies present in the blood than typical, it can be a sign that the body is attacking itself.
Since rheumatoid factor can also come back positive in people who are fighting infections, or have other autoimmune conditions, rheumatologists also check anti-CCP levels, since this test is more specific than rheumatoid factor and can help provide more information to your doctors.
Test results are considered seropositive when blood levels are elevated for rheumatoid factor or anti-CCPs, though not everyone with seropositive test results will have symptoms of rheumatoid arthritis, and there are some people who have other symptoms of rheumatoid arthritis who have no antibodies in their blood (i.e., 20-25% of people with symptoms will have a seronegative test result). Before making a diagnosis, your doctor will also evaluate the symptoms you have in addition to your blood test results.
Someone who has seronegative test results may still be diagnosed with rheumatoid arthritis based on their symptoms. However, individuals who are seropositive have a higher chance of having inflammation affecting other parts of their body (e.g., lungs, skin) and may have a more aggressive form of the disease.
Knowing your test results will help your doctors understand which medications might work best to treat your symptoms.
Arthritis Talks Webinars
Arthritis Talks webinars on the latest guidance direct from arthritis experts to help you get more out of life with inflammatory arthritis.
 |
 |
 |
| Rheumatoid arthritis in 2016: Are we making progress? | Inflammatory Arthritis: What you need to know | Inflammatory Arthritis: Types and Treatments |
| Dr. Michael Starr explains rheumatoid arthritis, treatment options and the importance of early intervention… | In this Arthritis Talks webinar, rheumatologist Dr. David Robinson zeroes in on what you really need to know about inflammatory… | Dr. D. Robinson, Rheumatologist on osteoarthritis & inflammatory arthritis: rheumatoid, gout, psoriatic + more; dealing with pain… |
| View More Webinars |
Contributors
This information was last updated September 2023, with expert advice from:
Bindee Kuriya, MD, SM, FRCPC
Assistant Professor, Department of Medicine
Division of Rheumatology University of Toronto

