Introduction
Beyond professional services, becoming a caregiver for a person with arthritis is typically an informal process that arises out of necessity. Often people become caregivers when a loved one requires additional help and support. This may be because of a new diagnosis, health event, or worsening of symptoms that have been present for a while. No matter how you have come to be a caregiver, this guide is meant to be a resource to you in providing care for your loved one with arthritis. It includes an overview of:
- The basics of caregiving
- Information about arthritis
- Arthritis treatment options
- Tips on how to approach difficult conversations
- Respectful relationships and power dynamics in caregiving
- Worksheets to help plan your time and provide care
- As well as a section about self-care for you as the caregiver
“Be kind and patient, maintain a person’s dignity and treat them as you would want to be helped or cared for. Caring and helping someone at a very difficult time in their life is not just a job. It is an act of love and kindness for a fellow human being who very well could be you one day.”
– Person living with arthritis
Introduction to Caregiving
Caregiving is the act of providing help and comfort to another person. It can involve many different activities, such as grocery shopping; help with dressing, eating, toileting; or providing emotional support to another person while they navigate a physical, emotional, or health challenge.
When discussing caregiving practices, often we hear about caring for children or older adults, though people of all ages may require support from a caregiver.
Caregiving can be a short-term role, or it can be something that lasts a very long time depending on the needs of the care recipient, as well as your own needs and abilities to provide care.
Although some people may have multiple health conditions contributing to their need for care, the term ‘Caregiving’ in this resource will refer to activities associated with the act of providing care for someone with arthritis.
What Is Arthritis?
Arthritis is a term used to describe a group of over 100 diseases characterized by inflammation in the joints or other areas of the body. Arthritis is a disease and not a natural part of aging. It can affect anyone at any age.
Symptoms of arthritis can range from mild to severe. Most people with arthritis experience chronic pain, fatigue, restricted mobility, lowered mood and other symptoms that can combine to reduce their quality of life.
Arthritis can involve almost any part of the body. The joints most often affected by arthritis include the hip, knee, spine or other weight-bearing joints, though it can also affect non-weight-bearing joints such as the fingers.
Arthritis is a chronic condition: it affects people on an ongoing, constant or recurring basis over months, years, or even a lifetime. Currently, there is no cure for arthritis, but there are strategies to manage the disease.
Arthritis Types: Arthritis is often divided into two categories – Inflammatory Arthritis (IA), and Osteoarthritis (OA).
Osteoarthritis (OA) is the most common form of arthritis and it affects more Canadians than all other forms combined. It is a progressive disease of the whole joint that leads to breakdown of joint cartilage and the underlying bone. Osteoarthritis is the result of the body’s failed attempt to repair damaged joint tissues. While joint damage can occur through deterioration over time, it can also occur in response to an injury or due to differently formed joints. While the underlying process of OA cannot be reversed, the symptoms can often be relieved or significantly improved with lifestyle measures and medications.
To learn more about Osteoarthritis, visit our OA Resource Hub.
Inflammatory Arthritis (IA) encompasses a number of different conditions. Most forms of IA are also autoimmune diseases, where the immune system – the body’s defense system against infections and other invaders – mistakenly starts to attack the body’s own healthy tissues. With IA, the source of joint damage is from inflammation rather than from a wearing away of cartilage.
There are many different forms of inflammatory arthritis. The most common forms of IA include rheumatoid arthritis, ankylosing spondylitis, and psoriatic arthritis. Early diagnosis and regular treatment are important to slow disease progression, limit joint damage and reduce symptoms.
To learn more about Inflammatory arthritis, visit our Arthritis A-Z resource page.
Treatment Overview
While there is no cure for arthritis, there are many different treatment options available. Not every treatment option will be appropriate for everyone with arthritis. There are also many drug-free pain management tools available to provide pain relief in addition to lifestyle modifications.
Regular physical activity, including therapeutic exercise, has numerous benefits for people living with arthritis, both physical and psychological. Eating a balanced diet is also recommended to help maintain good health. For people with arthritis, keeping up with exercise routines can feel like a chore and may not feel enjoyable, especially if movement causes pain or discomfort. However, movement is key to maintaining mobility and range of motion.
As a caregiver, being able to encourage exercise and movement will help your loved one stay active. Plan regular walks or exercise routines in your daily schedule. Make it a fun activity you can do together. If it is difficult to get outside due to mobility concerns or bad weather, consider alternatives, such as playing interactive video games that encourage movement. Visit Arthritis Society Canada’s 20-Minute Warm Up for the Joints video that can be done while seated, or exercises for osteoarthritis, many of which can be done seated or while lying down. People with inflammatory types of arthritis may need to take it easier during a flare, but they can still continue with range of motion exercises.
Your loved one may be taking medication to help manage the symptoms of their arthritis. Some medications have undesirable side effects, such as nausea, which may impact a person’s appetite or ability to eat. As a caregiver, it is important to understand how these medications may impact your loved one’s ability to participate in daily activities. Use our medication guide to learn more about different arthritis medications. If your loved one is experiencing negative side effects, or is having difficulty managing their symptoms, it is always best to check with their doctor or pharmacist before making any changes or stopping any treatments. It is also important to check with a person’s doctor or pharmacist before administering any new medications to them, including non-prescription medications such as pain relievers or natural supplements. Some arthritis medications might interact with other drugs or supplements.
To help keep track of the medication your loved one is taking and when it was last administered, consider using a medication chart.
Depending on the level of your involvement in providing care, it may also be helpful to support your loved one in creating a medication history to be used for medical appointments, hospital visits, or any time a more thorough medication history may be required. It can also help keep track of symptoms, and how they have changed over time.
Be mindful that not everyone will want their caregivers involved in their medication care, or in knowing which medications they are taking. Some people also take medications for reasons other than arthritis, and may not want to share this information with you. Remember to take the lead from the person you are caring for, and let them decide what information to share with you.
Medical Appointments
Part of on-going care for chronic health conditions like arthritis includes regular medical appointments and check-ups. The frequency of appointments will vary depending on each person but knowing what to look out for as a caregiver can help provide vital information during an appointment.
Not everyone will want their caregiver to be in the room during an appointment, so be sure to have a conversation ahead of time with your loved one about what they may want.
If all your loved one needs from you is help getting to and from the appointment, respect the boundaries they have set. Offer observations and suggestions only if they are welcomed.
If your loved one does want you in the room, discuss ahead of time what you can do to be helpful. You could take notes, ask questions that you prepared ahead of time, help remind your loved one to ask the questions they have written down, or be a source of emotional support as a listener and let your loved one do the talking.
There are some things that you can do to help your loved one prepare for appointments ahead of time, to make the most of the time they will have with their practitioner.
Use the Appointment Checklist and Symptom Tracker to help your loved one keep track of any changes that occur between appointments. Using a Medication Tracker or Medication History Log may also be helpful, especially in communicating side effects or a change in symptoms.
Forms of Caregiving
Formal caregiving is the term used to describe people who are paid for their services and have received formal training and education in providing care. Some formal caregivers are licensed and regulated by a regulatory body, such as nurses. Formal caregivers may come into your home through a home care program or provide respite care at an overnight facility or long-term care residence.
Informal caregiving is the term used to describe a person who provides care for another person outside a professional care context. Usually, they are closely connected to the person receiving care. This could be an immediate family member, spouse or partner, a parent, an adult child, friend, or someone known to the person receiving care. There are also informal care collectives that may involve others in the caregiving relationship.
Informal caregiving plays a vital role in how an individual receives care. Often, informal caregivers are present for daily tasks that are an essential part of a person’s care. Some of the tasks you may take on could include:
- Preparing or cooking meals
- Household chores (laundry, cleaning, dishes)
- Driving to and from appointments
- Providing help with toileting activities
- Providing help with bathing
- Provide help with dressing
Informal caregiving care takes on many forms outside of providing basic needs too. This could include:
- Being a support for your loved one when they need to express their feelings or talk about what’s bothering them
- Going for a walk, or exercising together
- Watching a movie, or sharing a hobby together
- Being a source of emotional support and friendship
Many people receive care from informal caregivers, or a combination of caregivers, with formal caregivers providing respite for the informal caregivers.
Caregiving Relationships
Caregiving is sometimes thought to be a one-way transaction, where the person receiving care is assumed to be the only person benefiting from the relationship. This isn’t usually the case. Typically, caregivers receive mutual support, emotionally or otherwise, from the person they provide care for. It may be helpful to think about your own situation and all the reasons why you want to help provide care for your loved one, and what you also receive in return.
Even though the person receiving care needs help some or all of the time, they can still provide love, care and support to their caregivers too. This is especially true if you as the caregiver are a partner, spouse, close friend, or family member.
“Caregiving is emotionally and physically taxing, but there is great benefit and joy in the mutuality of caring and being cared for”
– Person providing care
Although some people may view caregiving as an obligation, most people provide care because they want to help those they love and care about to thrive and be a part of their lives. When people view caregiving as an obligation this can cause tension or resentment in the relationship.
Relationships with close friends and family can become complicated when caregiving is involved. If the person receiving care experiences a sense of loss or a shift in the way they perceive their place in the family, relationship dynamics may also change.
“You don’t need dependence on someone you need to be treated in a way that maintains your independence and dignity. Nobody wants to rely on others for tasks they feel they should be able to do on their own…”
– Person living with arthritis
It’s important to keep in mind that even though your loved one needs care and support, they still have the final say about what happens to their body and in their care.
Receiving care may leave your loved one feeling exposed, or vulnerable. For many people, adjusting to a need for care can be difficult. For example, a parent might feel embarrassed about suddenly needing help from an adult child, or a spouse or partner may not want to be viewed differently in their relationship. It is important to respect their wishes and provide care in a way that will help your loved one remain as independent as possible, without shaming them or treating them like a child.
“…arthritis really does change day to day, from pain levels to pain location. that we really don’t want to be in this position, we want to be more active and pain free and do not want to be a burden to those around us. we get very frustrated and did not expect to be in this position, particularly at this point in our lives. we feel guilty about the pressure we add to those around us and also appreciate that there are many others who suffer far more with poor health issues which can make us feel like ‘whiners’ and even worse.”
– Person living with arthritis
When a loved one is experiencing things beyond our control, such as a pain flare or difficulty with movement or daily tasks, it may bring up all sorts of different emotions for you as an important person in their life. You may want to do things for them or try to fix the situation with tangible solutions. While the help may be well-intended, this could lead to feelings of frustration for the person experiencing pain or difficulties. At the same time, not knowing how to improve the situation could lead to a sense of helplessness for you.
During times when you feel helpless, it’s good to be able to recognize this, and take a step back when you need to.
Burnout and Self-Care
Let’s take a moment to talk about burnout. Burnout is a feeling of emotional, physical, and/or psychological stress caused by repeating the same type of stressful activity over and over. It might not feel like a bad type of stress because you are helping someone you love, and you may not even recognize signs of burnout when they start. Burnout can happen without even noticing it, which might feel sudden and even more overwhelming when this happens.

What can you do to prevent burnout?
- Maintain social networks
- Keep physically active
- Stay involved in or take up a new hobby
- Take breaks away from repetitive tasks
Caring for another person can be very time-consuming and emotionally taxing. It’s important to set aside time just for you so you don’t feel overwhelmed. Below are some tips to help manage stress and burnout, including self-care practices.
- Journaling
- Engaging in personal hobbies and activities
- Making intentional time for self/taking time out
- Mindfulness
- Meditation
- Social supports, and/or therapy
- Sleep
- Eating well (consistent, balanced meals, spaced throughout the day)
- Managing own health needs – prioritizing personal health needs to be best able to help someone else (when possible)
- Create or maintain a routine/schedule
- Plan ahead, but prepare for the unexpected
- Schedule respite care so you can have dedicated time to yourself
Self-care can take on many different forms. It could be as simple as taking a half hour to yourself to read a book, go for a walk, or watch a favourite show uninterrupted.
Self-care could also involve taking a more significant break from care, such as a day or two out of your weekly schedule to visit with friends or family or spend a night away. It could include taking a class or working on a hobby while someone else takes over primary care during a set time each week.
During times when it is difficult to leave your home, consider attending an online class or event. Many options are available through local continuing education programs, libraries, or community centres.
For caregivers who provide more around the clock care, taking larger, more significant breaks away can help break up your schedule and reduce the amount of stress build-up from being the constant source of support for everyone else.
It is very important to build up and maintain your own social support networks, separate from the person you provide care for. As people grow older, it can sometimes feel more difficult to maintain or form new friendships. In order to provide care for someone else, it is essential that you are able to practice social well-being.
If you are struggling to think of people you can call to talk to or enjoy an afternoon out with, try connecting to others through online forums, community centres, signing up for a class, or joining a club or volunteer activity. You may also find it helpful to join a caregiver support group or connect with a mental health professional. Your doctor might be able to connect you to a social worker or psychiatrist funded by your government health plan, or there may be free counselling services you can access in your region or online.
Visiting www.211.ca or calling 211 on your phone can help you learn about services available in your area.
A large part of self-care is prioritizing your own needs, so that you have the capacity to care for others without feeling overworked. Ensuring you have regular breaks will also give you and your loved one each something new to talk about when you return to providing care.
National Resources
Carers Canada
British Columbia
Family Caregivers of British Columbia
Alberta
Caregivers Alberta
Saskatchewan
Caregiver Information and Support: Saskatoon Council on Ageing
Manitoba
Caregiver and Family Supports: Manitoba Health, Seniors and Long-Term Care
Ontario
The Ontario Caregiver Organization
Ontario Caregiver Coalition
Quebec
L’appui
New Brunswick
Social Supports New Brunswick
New Brunswick Caregiver Guide
Prince Edward Island
Prince Edward Island AccessAbility Supports
Nova Scotia
Caregivers Nova Scotia
Newfoundland and Labrador
SeniorsNL: Brochures for Caregivers
Yukon
Yukon: Resources for Caregivers
Northwest Territories
Northwest Territories Caregivers Guide
Respite Care and Communication
 Respite care may be another option to consider if the person you provide care for requires a significant amount of care. Respite programs may involve a fee and can vary by location and need. Some regions offer day away or afternoon programs for people requiring care to get out and socialize in a different setting while their caregiver can use that time to do other tasks or have time to themselves.
Respite care may be another option to consider if the person you provide care for requires a significant amount of care. Respite programs may involve a fee and can vary by location and need. Some regions offer day away or afternoon programs for people requiring care to get out and socialize in a different setting while their caregiver can use that time to do other tasks or have time to themselves.
External help, respite care, or home care workers are all different options to help you as a caregiver have a break to practice your own self-care. Be mindful that some forms of respite care will work better than others depending on the level of care needed by your loved one.
Not everyone will feel comfortable with a stranger coming into their home or providing care for more personal hygiene needs. However, others may feel more comfortable with someone they don’t know coming in to help with hygiene care. Talk with your loved one to determine what type of respite care makes the most sense for your situation. Come up with a list of tasks and questions you each think would be most helpful to discuss with a respite program or care provider, and make sure to ask if they can provide this type of help.
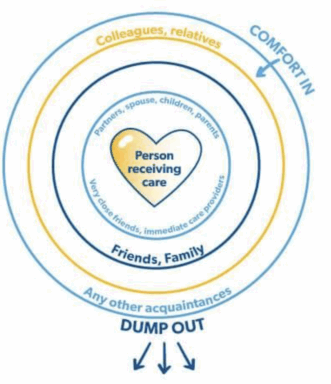 Consider the concept of dumping out and comforting in, which places the person receiving care at the centre of the care circle, and everyone else in their life is on a ring surrounding the circle. Some people will be on rings closer to the centre, while others will be further out, depending on how close of a relationship they have to the person receiving care. Dumping out means that the person in the centre can vent to anyone they want on any layer of outer rings, and the people on the next closest ring can dump out their feelings and vent to anyone else on a ring outside their own, but it’s not appropriate to dump feelings of frustration back into the circle. Comfort is provided inward, and venting dumped outward.
Consider the concept of dumping out and comforting in, which places the person receiving care at the centre of the care circle, and everyone else in their life is on a ring surrounding the circle. Some people will be on rings closer to the centre, while others will be further out, depending on how close of a relationship they have to the person receiving care. Dumping out means that the person in the centre can vent to anyone they want on any layer of outer rings, and the people on the next closest ring can dump out their feelings and vent to anyone else on a ring outside their own, but it’s not appropriate to dump feelings of frustration back into the circle. Comfort is provided inward, and venting dumped outward.
Just because your loved one is the centre of the circle for their arthritis and other care needs, it doesn’t mean that you also won’t be in the centre of your own circle at times, and your loved one will be there to help support your needs and provide comfort to you when you need to vent. However, making someone feel guilty for the arthritis care they are receiving and the burden it places on the caregiver is unfair to the person receiving care, whether intentional or not.
Being a caregiver doesn’t mean you always have to be present for all aspects of caregiving. It’s actually really important to know your own limitations for providing care. Some people are great at providing bathroom support, but don’t like the idea of doing dishes. Someone else might really enjoy cooking meals and helping with cleaning chores but doesn’t feel as well-equipped to help someone get dressed. Everyone will be different, and your limitations and abilities will not necessarily be the same as those of someone else.
It’s okay to not want to take on every task, and in fact it’s really helpful to be able to say, “actually, this doesn’t feel okay to me” when reflecting on your own boundaries. When people take on tasks that make them feel uncomfortable, or easily frustrated, they are more likely to experience burnout, or caregiver fatigue. This can also lead to tension between the caregiver and person receiving care, which can be upsetting for everyone involved.
It is important to take the time to have open conversations with the person you care for, as well as other people helping to provide care. Creating a schedule of tasks for each person to take on can be a helpful way of ensuring everyone feels supported in providing care.
If you are the only person providing care, take some time to write out all the tasks that make you feel uncomfortable, or anxious, and talk with the person you are caring for to decide on a plan that helps you help them. For each task that you are not comfortable, or able to help with, it is essential that this care still be provided. Use external agencies, the help of friends, family, or other support people to arrange for this care.
Depending on where you live, some community services provide low or no-cost support to seniors and/or people with disabilities. Visiting www.211.ca or calling 211 on your phone can help you find services available in your area.
Sometimes just talking about your concerns or anxieties around certain caregiving activities can be helpful too. If you have concerns you would hurt someone if you were helping them get dressed, discussing this openly could lead to a plan to make sure the person you are caring for is leading the process and can stop things if they don’t like how it’s going. There may also be assistive devices available that can make certain tasks easier. For example, installing grab bars in bathrooms or using a raised toilet seat might make toileting and bathing easier for some people. Adaptive clothing might enable greater independence while getting dressed. Visit the Arthritis Society Canada’s Assistive Devices Tool for further information and suggestions.
**Important**
While it is important to recognize your own boundaries and limitations in being able to provide certain types of care, this does not mean that this care can go unprovided. It is essential that all care needs are met. If you are not able to provide certain types of care, it is essential that those tasks are met through other care services, family, friends, or others in your circle of care.
Not providing a certain kind of care, or arranging for that care need to be met is considered neglect, and can leave your loved one in an unsafe situation, and negatively impact their health and wellbeing.
To help prevent frustration in your caregiving relationship, try having open and honest conversations about how you both feel. If you are not sure about something, instead of making assumptions about what your loved one wants, ask them to confirm that you have understood them correctly. Sometimes repeating a person’s words back to them can help clear up any miscommunication, and acknowledge you heard and understood them.
What I understand you are saying is that you need _________ and you would like me to stop _______. Did I understand correctly?
Most people don’t like losing a sense of independence, so talk about how you can help them maintain as much of their independence as possible, while still helping them get what they need.
You can use things like a caregiver task list to help guide your conversation about what tasks you can do to provide support.
If there are multiple people providing care, talk about what tasks feel most suitable for each person. Create a schedule so you know when each person will be available to take on those tasks, and to give everyone a sense of direction and accountability.
It can be difficult for some people to accept that they need extra help or care. Having a schedule with dates, times, and the name of the person doing each task can help to alleviate some uncertainty and anxiety that may arise for the person receiving care. It gives everyone a shared understanding of what to expect.
Below is a sample care chart for Nadine, who needs around-the-clock support. Nadine’s partner Carrie is her main support person and is present throughout the week. On weekends, their son James often takes over, with their granddaughter Hannah helping out. Hannah also comes over during the week to watch movies, help prepare meals for the next day and go for walks. Nadine and Carrie’s friends Lauren and Xu come over to help when they can, and a personal support worker (PSW) also comes into the home three days a week to help with care.
In this sample chart, each person has been assigned a colour. When the chart uses their colour, it means they are the person physically present to help when needed, and the text is used to highlight a specific piece of care, or activity.

Consider using a spreadsheet or chart program to create your own caregiver schedule. Online platforms can be shared right to a phone or tablet, emailed, or printed out for everyone to see.
Scenarios
In this module, we’ll explore different ways to respond to care needs that may be beyond what you are able to provide.
It’s important to know your own limitations as a caregiver. There will be some tasks that you may find easier or more enjoyable and others that might make you feel uncomfortable.
If you have been asked to help with bathing, how might you respond?
- “Sure, that’s no problem. Would you like me to help you get undressed, or would you prefer I enter after you are already undressed?”
- If helping with bathing is a task you are comfortable helping with, this is a good response. It also allows an opportunity for your loved one to decide how they want to approach their bath.
- “I hear that you need help with bathing. This isn’t something I feel comfortable helping with. Is there someone else we can ask to help you with this?”
- This is a good example of expressing boundaries, but remaining open to still helping your loved one get what they need. Work together to find someone who can help with bathing.
- “You don’t need a bath tonight, how about I help you to bed instead?”
- Instead of telling someone they don’t need something, try to express that helping with bathing makes you uncomfortable, and try to find a solution that works for both of you.
You’ve been asked to help prepare meals. The person you provide care for eats meat, and you are not comfortable preparing meat. How do you proceed?
- “I’ll cook for you, but only vegetarian meals.”
- This may be okay with the person you are caring for, but it may not. Always ask to confirm they are okay with what is being prepared. If you can’t stick to the meal plan, consider helping another way .
- “I see on the meal plan this week is a dish with chicken. I’m not comfortable preparing meat, but I would be happy to help prepare any non-meat dishes.”
- If you know you are not comfortable preparing meat dishes, plan ahead and be clear that this isn’t something you are comfortable doing so you will not be stuck figuring our meal changes last minute.
- “I really don’t like cooking, is there another way I can be helpful?”
- Its okay to take up other roles instead. Check in with the person you care for to make sure there is someone else who can help with cooking. If not, come to a solution to get more help so they can eat.
While helping Ahmad get dressed, a glass of water accidentally spills on the floor. You immediately grab a towel and start mopping it up, but notice Ahmad’s walker is blocking you from half of it. How do you proceed?
- You casually move Ahmad’s walker out of the way, and continue mopping the water up. When putting the towel away, you forget to move his walker back.
- While it may have been unintentional, it’s always important to ask permission before moving an assistive device. Its also very important to never leave someone stranded away from their device.
- You ask Ahmad if he can move his walker out of the way so you can mop the rest of the water. He does so, and moves it back into place.
- If the owner of the assistive device is able to move it themselves, this is preferable, though it may not always be an option. If they are unable to move it, ask permission to move it yourself.
- You ask Ahmad if you can move his walker to mop up the remaining water on the floor, and then promptly move the walker back where it was.
- Asking to move any assistive device is important, as this is a form of access to movement. Taking away the ability of someone to move independently is not okay. Always move a device back when possible.
Caregiving can be challenging in many different ways. One challenge that can sometimes arise in caregiving relationships is something called power dynamics. Power dynamics describe the power in a relationship between two or more people. Often a person who is able to make decisions for another, take action or inaction that will affect someone else, or who can influence the behaviour and actions of others is considered to be in a position of power.
Positions of power are not always negative, like when a parent uses their influence over a young child to protect them from a harmful situation. It is important to understand that anytime someone is reliant on care from another person there will be a power dynamic in that relationship.
It can be difficult to discuss power dynamics, but it is important for caregivers to be aware that some forms of power dynamics can be very unhealthy and unhelpful to loved ones. In this section we’ll explore some of the ways power can change or influence caregiving relationships.
Often in caregiving relationships, situations can arise where the care provider is also organizing and helping to coordinate many areas of their loved one’s life. This could include helping to support hygiene needs, meal planning, scheduling, or paying bills, as well as coordinating support from others.
It is very important to remember that even though you may be providing care as a caregiver, the person receiving your support should be the person in control of these vital areas.
When all control falls onto the care provider, it is very easy to make changes to suit the care provider’s needs without giving consideration to what is best for the person receiving care. This power imbalance can lead to unhelpful and unhealthy actions that can unintentionally harm your loved one.
To help combat power imbalances, regularly check in with your loved one around what they need and want in each situation. Don’t assume because you asked once that the answer will be the same next time.
It can be helpful to set aside a scheduled time each week with your loved one to check in about how things are going and to talk over any changes either of you would like to make. Making this set appointment will give you each an opportunity to discuss what is working well and what could be improved. It can help to de-personalize this process and focus specifically on care needs. If there is more than one caregiver involved in providing care, invite them to these regular check-ins also, or find a way to check in separately, or update them on any changes each week. This way everyone stays informed, and it takes the guess work out of what is needed.
In speaking with people who receive care for arthritis, the most common areas of concern were about caregiver conduct and wanting to ensure a safe and healthy environment to live free from harm. This section focuses on different forms of power imbalance and ways to identify and address potential areas of concern in your caregiving relationships.
Manipulation can take on many forms and can be exercised both by the care provider and the person receiving care. Sometimes when people are dependent on another person for care, they may use forms of manipulation such as guilt or threats to ensure they are able to get the things they need to survive and to maintain function. Often this is not intentional, though it can still be harmful to the care provider, who needs to maintain boundaries and limitations to ensure they are able to continue providing care.
When a caregiver uses manipulation or guilt to try and get their loved one to do tasks in a specific way, or to refuse a caregiving task, this is a form of unhealthy behaviour, and a potential sign of burnout.
Shaming someone is another form of an unhealthy behaviour, and can come from either the care provider or care recipient. Shaming others, especially for things beyond their control is never okay, especially from those who control access to the items the person may be shamed for – such as a caregiver shaming their loved one for clothing looking shabby when they were dressed by their caregiver.
Gaslighting is a form of manipulation. It is often used by an individual or group to make someone question their choices, second guess their memories, and doubt or question their judgement. It can also include convincing someone that their needs are not important.
Gaslighting often comes about when people are trying to gain a sense of control over a situation. It can happen without realizing it, especially if things in your caregiving relationship feel out of control, or unpredictable. A common example of gaslighting is saying something negative, or insulting to someone, only to then tell them that they are wrong, or foolish when they try to defend their stance.
Another example is setting someone up to answer a question in a particular way, and then demean them when they answer as anticipated.
Example
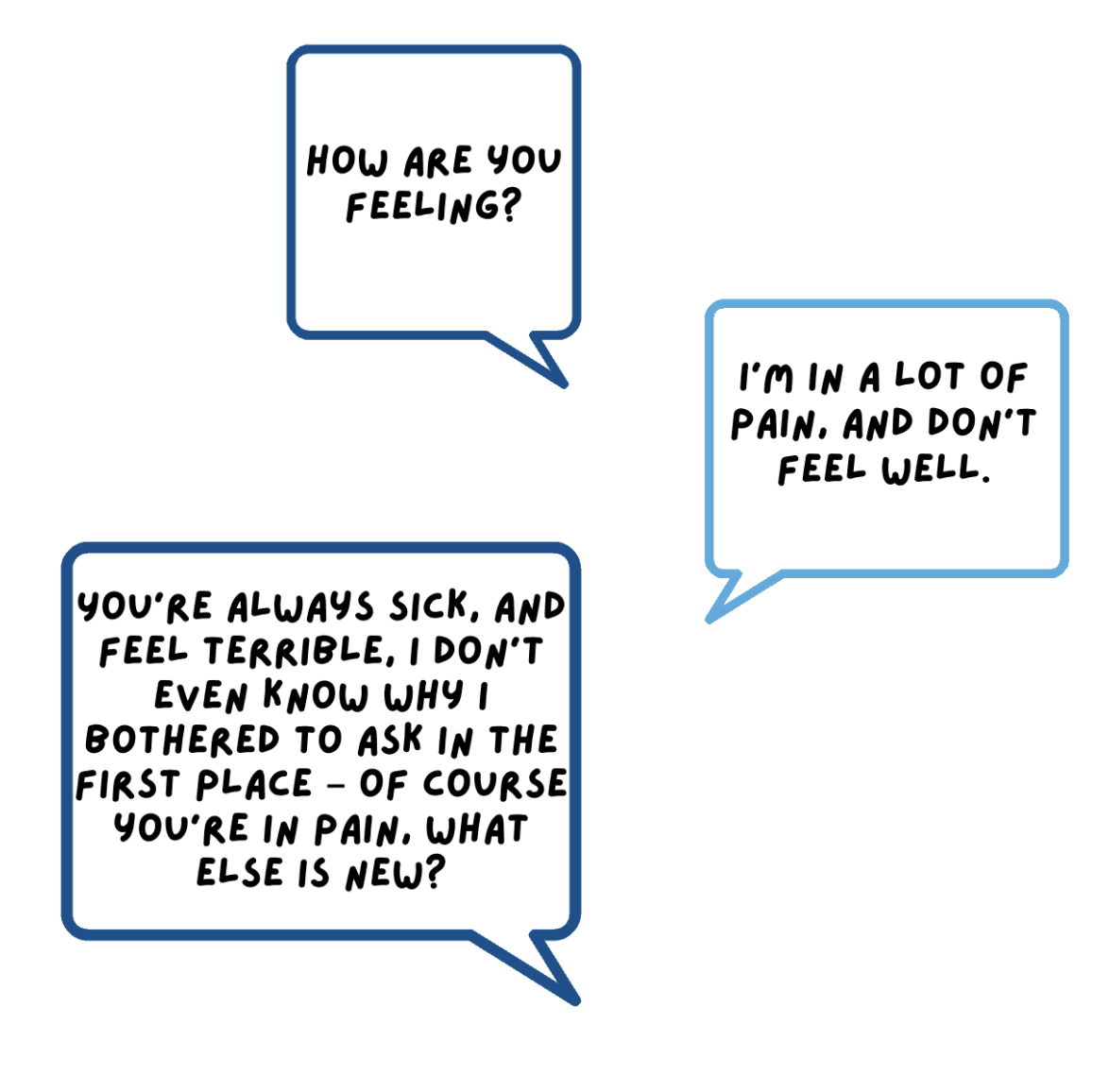
If you are concerned about the type of power dynamics you may have with your care recipient, seek external help.
- Ask for guidance from either your loved one’s medical care providers or your own, a social worker, psychologist, or home care case worker.
- Talk with friends and your own social supports to vent your frustrations outside of providing care.
- Seek respite options to help in providing care.
Respite is a form of additional help or care provided by external help, or having your loved one spend a few hours at a day program, days or even a few weeks in a residential program to allow you time to have a break and recuperate. Providing care on a full-time basis can be quite exhausting, and it is important to have breaks to maintain your own health and wellbeing.
If people in your care circle are behaving this way, try to talk with them about taking a break from caregiving. If you are not sure about the impact this will have on your loved one’s care, check in with them about how their care has been going, and the things you have been noticing from their other care providers.
If you feel that you may sometimes act this way, or say something similar to your loved ones, it’s important to seek support from a counsellor, or support person who you can talk with. This is not healthy behaviour, and being able to find support for yourself will also help to support your loved one.
If you are approached about your own behaviour by another caregiver on your loved one’s care team, try to acknowledge their concerns, and respond in a way that will best serve your loved one. Everyone brings their own unique experiences to caregiving, and the ultimate goal is to help your loved one to live more comfortably. If actions and behaviour by you or anyone else are negatively impacting this, then it is necessary to take a step back to assess what can be done next. Reaching out to your local 211 service, or community health centre can be a good place to start.
Frequently Asked Questions
Every person is different so this will vary based on the person you are caring for, but some people with arthritis may have difficulty with mobility, or others with standing for longer periods of time. If they can no longer hold knives to chop vegetables, or grip to open jars or cans, they may need assistance with setting up their kitchen to be more accessible so they can still cook with the help of some assistive devices for the kitchen.
Others may need more help with daily tasks such as dressing or using the bathroom. Adaptive clothing and assistive devices may help a person perform some dressing or toileting/bathing tasks on their own, but it is important to ensure that support is available if needed, whether it is you or another caregiver providing this support. Depending on the level of care needed, caring for a person with arthritis could mean helping out for a few hours each week, or it could involve 24-hour care. Some people with arthritis who need care also have other conditions that require caregiving support, which may increase the amount and type of support they need.
It’s always best to ask the person who needs support what would be most helpful to them, and how you can provide that support in a way that feels affirming and caring to them.
Help can come in all kinds of forms. It’s important to recognize that receiving care from another person can be a vulnerable experience. Even if you have a close relationship with someone, it doesn’t mean they will feel comfortable with you seeing them in a vulnerable state. There are many ways you can still be a part of their life or provide help.
Talk to them about ways you can still be a part of their life and ask how you can help support them. They might really want you around for other elements of their day-to-day activities (ex. as an exercise pal), but may not want you involved in bathing them, or cooking meals.
If you do ask how you can help and they still respond that they don’t want you directly involved in their care, respect this decision, but let them know you are available if they need your support. Transitioning to care giving/receiving can be a very difficult process for all involved.

